North Texas Research Forum 2026
Files
Download Full Text (607 KB)
Division
North Texas
Hospital
Medical City Arlington
Specialty
Internal Medicine
Document Type
Poster
Publication Date
2026
Keywords
acute hyperammonemia, anoxic brain injury
Disciplines
Internal Medicine | Medicine and Health Sciences | Pathological Conditions, Signs and Symptoms
Abstract
Background: Acute hyperammonemia presents as a toxic state with the clinical presentation as altered consciousness, seizures, and coma. Hyperammonemia disrupts astrocytes osmotic balance via glutamine accumulation, triggering brain edema, inflammation, and apoptosis whom mechanism is closely parallel to hypoxic ischemic injury. This overlap necessitates differentiating metabolic causes from hypoxic etiologies, as timely ammonia clearance therapies can prevent catastrophic outcomes. This case underscores the need for close clinical vigilance and early recognition of severe hyperammonemia
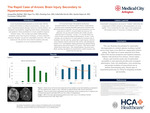
Case Presentation: A 65-year-old woman with metabolic dysfunction-associated steatotic liver disease related cirrhosis complicated by recurrent ascites requiring bimonthly paracentesis presented with abdominal distension and pain. Her most recent paracentesis was two weeks prior in which 5L of ascitic fluids was removed. On admission, she was alert and oriented with a mildly elevated ammonia level of 58 µmol/L. On day 2, 4L of ascitic fluid were removed with concurrent albumin administration. On day 3 in the morning, she was placed on 4L nasal canula for increased work of breathing. Later the same day, patient had a rapid response called for acute respiratory distress and seizure-like activity, and subsequently, transfer to ICU and intubated. Repeat ammonia level obtained during rapid response showed increased to 975 µmol/L. MRI head revealed global anoxic brain injury. After multidisciplinary discussion and a family meeting, the patient was transitioned to comfort measures and expired later on the same day.
Lessons Learned: Catastrophic consequences can occur in “routine” admissions for compensated cirrhotic patients as decompensation can occur rapidly. Close monitoring for early signs of decompensation with prompt actions is necessary to mitigate mortality.
Conclusion: This case illustrates the potential for catastrophic decompensation in cirrhotic patients resulting in global anoxic brain injury in an otherwise compensated cirrhotic setting. The rapid rise of serum ammonia level likely reflects both increase production and impaired clearance. Patients with advanced liver disease, chronic kidney disease, and recurrent ascites may be particularly susceptible to such ammonia elevation and consequent deterioration. Early risk stratification, close monitoring, and prompt escalation of neurocritical care in patients demonstrating early clinical signs of hyperammonemia may be critical in mitigating morbidity and mortality.
Original Publisher
HCA Healthcare Graduate Medical Education
Recommended Citation
Bekhit, Jacqueline; Vu, Ngoc; Xue, Jiaming; David, Gabriella; and Sajawal, Qasim, "The Rapid Case of Anoxic Brain Injury Secondary to Hyperammonemia" (2026). North Texas Research Forum 2026. 20.
https://scholarlycommons.hcahealthcare.com/northtexas2026/20