North Texas Research Forum 2026
Files
Download Full Text (563 KB)
Division
North Texas
Hospital
Medical City Arlington
Specialty
Internal Medicine
Document Type
Poster
Publication Date
2026
Keywords
esophageal leukoplakia, epidermoid metaplasia, plaques, premalignancy
Disciplines
Digestive System Diseases | Internal Medicine | Medicine and Health Sciences | Neoplasms
Abstract
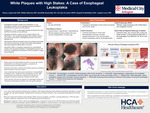
Introduction: Esophageal leukoplakia, also termed esophageal epidermoid metaplasia (EEM), is a rare esophageal epithelial disorder characterized by keratinized squamous plaques on esophagogastroduodenoscopy (EGD). With a prevalence of < 0.5%, it is often incidentally identified during evaluation for nonspecific upper gastrointestinal symptoms. EEM is considered a premalignant condition due to its association with esophageal squamous cell carcinoma (SCC), yet management and surveillance strategies remain undefined.
Case Presentation: A 65-year-old woman with hypothyroidism, hypertension, hyperlipidemia, and remote aplastic anemia treated with bone marrow transplantation 35 years prior presented with chronic cough and progressive dysphagia to solids and liquids. She denied tobacco, alcohol, or illicit drug use. No weight loss, abdominal pain, or blood in stool was noted. CT of the neck with contrast revealed curvilinear mucosal hyperenhancement involving the mid to distal thoracic esophagus without lymphadenopathy. Physical examination and vital signs were unremarkable. EGD revealed a ringed esophagus with diffuse and localized mucosal abnormalities in the mid-esophagus, initially concerning for eosinophilic esophagitis. Histopathology demonstrated low-grade squamous dysplasia on random biopsies (BX) and high-grade squamous dysplasia on targeted mid-esophageal BX. Alcian blue and periodic acid–Schiff stains were negative. Immunohistochemical staining demonstrated increased Ki-67 proliferation index and positive p53 expression. The patient was initiated on proton pump inhibitor therapy. Repeat EGD at four-week follow-up demonstrated extensive white, lacy, scaly mucosa with granulation tissue involving approximately 80% of the esophageal circumference from 24 to 32 cm from the incisors. Repeat biopsies revealed extensive parakeratosis with full-thickness squamous dysplasia, without evidence of invasive malignancy, consistent with EEM. Given the rapid interval progression despite negative biopsies for invasive carcinoma, patient-physician discussion is essential to guide further management and surveillance.
Learning points: EEM is a premalignant squamous lesion with reported progression to SCC in approximately 25%. P53 is the most frequently implicated mutation, with additional alterations reported in PIK3CA, EGFR, MYCN, HRAS, and the TERT promoter. Although causality is unproven, associations with tobacco exposure, including second-hand smoke and alcohol use, have been described. Larger dysplastic lesions may benefit from endoscopic resection or ablative therapies such as radiofrequency ablation or argon plasma coagulation.
Conclusion: EEM is a precursor to SCC, and vigilant recognition is essential for early detection. Management includes addressing the underlying risk factors and focusing on individualised endoscopic surveillance of the area of leukoplakia as well as the surrounding background mucosa.
Original Publisher
HCA Healthcare Graduate Medical Education
Recommended Citation
Lapsiwala, Boney; Sharma, Ritika; Kasireddy, Karthik; Pavuluri, Devika; Prabhukhot, Rupali; and Awan, Amjad, "White Plaques with High Stakes: A Case of Esophageal Leukoplakia" (2026). North Texas Research Forum 2026. 23.
https://scholarlycommons.hcahealthcare.com/northtexas2026/23