North Texas Research Forum 2026
Files
Download Full Text (371 KB)
Division
North Texas
Hospital
Medical City Plano
Specialty
General Surgery
Document Type
Poster
Publication Date
2026
Keywords
trans-arterial embolization, TAE, gastroduodenal artery, GDA, gastrointestinal bleeding
Disciplines
Digestive System Diseases | Medicine and Health Sciences | Surgery
Abstract
Background Trans-arterial embolization (TAE) of the gastroduodenal artery (GDA) is a well-established and effective treatment for peptic ulcer bleeding and visceral pseudoaneurysms. Although generally safe, delayed migration or erosion of embolization coils into the gastrointestinal lumen is a rare but recognized complication that may occur months to years after the procedure. Proposed mechanisms include ischemic mucosal injury, mechanical pressure from the coil mass, and chronic inflammation. Clinical manifestations vary widely, ranging from occult bleeding and ulceration to perforation or gastric-outlet obstruction. Only a limited number of cases describing GDA coil erosion presenting with both bleeding and obstruction have been reported.
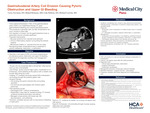
Case Presentation A 34-year-old man presented after a 20-foot fall. Initial trauma evaluation revealed no acute injuries; however, laboratory studies demonstrated profound anemia with a hemoglobin level of 3 g/dL. Following blood transfusion, upper endoscopy was performed and revealed active upper gastrointestinal bleeding with pyloric obstruction caused by a bundle of metallic wires. Review of prior imaging confirmed a history of remote GDA embolization, consistent with the endoscopic findings. The patient underwent exploratory laparotomy, which demonstrated erosion of embolization coils through the posterior gastric wall into the pyloric channel with an associated ulcer. The coils were surgically removed, and pyloroplasty with Graham patch repair was performed. His postoperative course was initially uncomplicated, and he was discharged on postoperative day seven. Two days after discharge, the patient was readmitted with nausea and vomiting. Cross-sectional imaging revealed a contained duodenal perforation and postoperative edema without evidence of an anastomotic leak. He was managed conservatively with bowel rest, nasogastric decompression, and intravenous antibiotics, resulting in full clinical recovery.
Lessons Learned
- Coil erosion is a rare but serious delayed complication of gastroduodenal artery embolization.
- Prior embolization should raise suspicion for coil migration or erosion in patients presenting with unexplained anemia, hematemesis, or gastric-outlet obstruction.
- Endoscopy and computed tomography are complementary diagnostic modalities, allowing visualization of intraluminal metallic foreign bodies and associated mucosal injury.
- Definitive management often requires surgical coil extraction and repair when endoscopic retrieval is not feasible or bleeding persists.
- Multidisciplinary collaboration among gastroenterology, interventional radiology, and surgery is critical for timely diagnosis and optimal patient outcomes.
Conclusion This case highlights a rare delayed complication of GDA embolization presenting with profound anemia and gastric-outlet obstruction years after the initial procedure. Awareness of coil erosion as a potential etiology is essential, particularly in patients with prior embolization and atypical presentations. Prompt recognition using combined endoscopic and imaging approaches, followed by definitive surgical management, can lead to favorable outcomes despite the severity of presentation.
Original Publisher
HCA Healthcare Graduate Medical Education
Recommended Citation
Newman, Corey; Rehman, Mahad; Beltran, Cody; and Carrick, Michael, "Gastroduodenal Artery Coil Erosion Causing Pyloric Obstruction and Upper GI Bleeding" (2026). North Texas Research Forum 2026. 42.
https://scholarlycommons.hcahealthcare.com/northtexas2026/42