Division
East Florida
Hospital
HCA Florida Kendall Hospital
Specialty
Internal Medicine
Document Type
Poster
Publication Date
2025
Keywords
electronic cigarettes, vaping-associated lung injury, EVALI
Disciplines
Critical Care | Internal Medicine | Respiratory Tract Diseases
Abstract
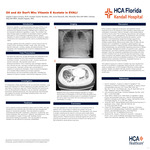
Introduction: Electronic cigarette or vaping-associated lung injury (EVALI) is an acute or subacute condition characterized by acute respiratory symptoms and bilateral pulmonary infiltrates seen in patients who are exposed to electronic cigarettes or vapes. The condition has been strongly linked to inhalation of aerosolized vitamin E acetate, particularly in THC-containing e-cigarette products. Despite regulation of vitamin E acetate in the production of electronic vapes, it continues to be a byproduct of EVALI due to counterfeit electronic vapes. Clinically, patients with EVALI present in various ways but are not limited to fever, shortness of breath, cough, chills, body aches, pleuritic chest pain, vomiting, nausea, and abdominal pain. Prompt recognition and management are crucial for mitigating adverse outcomes. Case Presentation: We report the case of an 18-year-old female who presented to the emergency department with initial complaints of progressive shortness of breath, nonproductive cough, vomiting, nausea and pleuritic chest pain. She reported recent use of tetrahydrocannabinol (THC) containing vape cartridges obtained from informal sources. Vital signs revealed tachycardia, tachypnea, and hypoxemia. Laboratory studies were unremarkable for infectious or autoimmune etiologies. Chest computed tomography (CT) revealed diffuse bilateral ground-glass opacities. Bronchoscopy with bronchoalveolar lavage (BAL) identified the presence of vitamin E acetate, confirming the diagnosis of EVALI. Investigations CT angiography initially performed to rule out pulmonary embolism. Lung fields were significant for diffuse bilateral ground-glass opacities with 5-year history of electronic vape use. Further infectious and autoimmune work up was performed to attempt to rule out vasculitis, eosinophilic pneumonia, bacterial pneumonia, and viral pneumonia. Bronchoscopy was negative for alveolar hemorrhage indicating further work up for possible vitamin E exposure. Treatment Due to patients worsening respiratory status while on HFNC, she was transferred to the intensive care unit where she was intubated and placed on mechanical ventilation. She was started on systemic corticosteroids 60mg BID, levalbuterol, ipratropium, budesonide, and empiric antibiotics with vancomycin, cefepime, and azithromycin. She was intubated for roughly 72 hours with moderate clinical improvement leading to extubation. She was educated on smoking cessation as well referred for pulmonary rehabilitation. Discussion: EVALI remains a diagnosis of exclusion with significant clinical implications due to its potential for rapid respiratory deterioration and multisystem involvement. Vitamin E acetate, a lipid-soluble additive commonly found in illicit THC-containing vape products, has emerged as a key agent in EVALI pathogenesis. Its interference with pulmonary surfactant leads to a chemical pneumonitis-like reaction, and its detection in bronchoalveolar lavage fluid strongly supports the diagnosis when aligned with clinical and radiologic findings. The condition predominantly affects young males under 35 years old and presents with a constellation of respiratory, gastrointestinal, and constitutional symptoms. Imaging typically reveals bilateral infiltrates, while histopathology may demonstrate organizing pneumonia or diffuse alveolar damage. Management centers on supportive care, systemic corticosteroids, and empiric antibiotics pending exclusion of infectious etiologies. Given the nonspecific presentation and overlap with more common conditions such as community-acquired pneumonia, a high index of suspicion and detailed vaping history are critical. Public health measures should continue to emphasize avoidance of THC-containing vaping products, particularly those from unregulated sources, to prevent recurrence and reduce morbidity. This patient’s exposure to vitamin E acetate may have resulted from the use of counterfeit or unregulated vaping products, which were widely circulated prior to FDA oversight of electronic nicotine delivery systems. Notably, the patient had easy access to these products through a family connection, as their father was employed/owner of a smoke shop. Conclusion: This case highlights the critical importance of considering EVALI in patients with a recent history of vaping who present with acute respiratory and gastrointestinal symptoms. The association with vitamin E acetate underscores the need for continued public health efforts, regulatory oversight, and education regarding the risks of unregulated vaping products. Patients should be cautioned against the use of such products and advised to avoid all forms of tobacco and vaping due to their potential to cause serious lung injury.
Original Publisher
HCA Healthcare Graduate Medical Education
Recommended Citation
Lopez-Lacayo, Angelo; Taylor-Bentley, Jordan; Masseli, Josef; Silva, Michelle; Diaz, Christy; and Zapata, Daniel, "Oil and Air Don’t Mix: Vitamin E Acetate in EVALI" (2025). East Florida Division GME Research Day 2025. 49.
https://scholarlycommons.hcahealthcare.com/eastflorida2025/49