The Annual HCA Fall Research Day on November 12th was a success, with a couple hundred virtual participants and attendees!
This forum continues to provide a high-level outlet for physicians and medical students to present novel contributions to clinical practice and medical knowledge. There were 223 presentations from 30 programs across 8 hospitals in the EFL division. Presentations spanned 7.5 hours over 4 virtual tracks and were arranged by specialty. Presenters had 5 minutes to present their posters orally, followed by 2 minutes of questions from the audience giving each presenter a chance to present their work orally and interact with the audience in real time. We were thrilled to see high levels of participation and engagement from the audience. The top 3 data-based and top 2 educational presentations were awarded.
-
Winners - Data-based
-
1st Place: Comparison of Diagnostic Accuracy of CT and SPECT-CT in Pseudarthrosis Detection: A Systematic Review and Meta-Analysis
Nicholas Schiller, MD; Miguel A. Cartagena-Reyes, MD; Elyette Lugo, BS; Diego Lopes De Lima, MD; Brett Schlifka, DO; Milad Alam, MD -
2nd Place: The Role of Bandemia in Clinical Outcomes of Critically Ill Septic Patients
Yerandy Gil, MD; Grettel Gonzalez Garcia, MD; Ambar Sekulits, MD; Rafael Miret, DO; Siddarth Kathuria, MD; Mauricio Danckers, MD; Daniel Heller, MD -
3rd Place:
Comparing ChatGPT and DeepSeek for Deprescription Support in Geriatric and Palliative Care: An Exploratory Study Using Clinical Vignettes
Gokhan Demir, MD; Angel Sanchez, MD; Sanaz Kashan, MD
-
1st Place: Comparison of Diagnostic Accuracy of CT and SPECT-CT in Pseudarthrosis Detection: A Systematic Review and Meta-Analysis
-
Winners - Educational
-
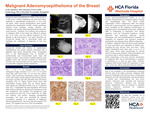
1st Place: Carcinoma with Osteoclast-Like Giant Cells, a Rare Histologic Variant of Breast Cancer
Robert Bender, MD; Makenna Bowman, MD; Matthew Lee, DO; Susana Ferra, MD -
2nd Place: The Face-Off Between Two Mimics: Lupus and Tuberculosis
Swati Swatisikta, MD; Nang Kham, MD; Ali Chaudhry, MD
-
1st Place: Carcinoma with Osteoclast-Like Giant Cells, a Rare Histologic Variant of Breast Cancer
-

National Outcomes of Pre-Emptive TIPS in Patients with Acute-on-Chronic Liver Failure and Variceal Bleeding
Aya Akhras, Waseem Wahood, Azizullah Beran, Bisher Sawaf, Asad Ur Rahman, David Goldberg, and Muhammed U. Shahid
Background
Pre-emptive transjugular intrahepatic portosystemic shunt (pTIPS), defined as placement within 72 hours of initial endoscopic therapy for an active variceal bleed, has been proposed as a strategy to reduce rebleeding and improve survival in high-risk patients with cirrhosis. We evaluated outcomes of patients with acute-on-chronic liver failure (ACLF) who presented with variceal bleeding and underwent therapeutic endoscopy (EGD) with or without the addition of pre-emptive TIPS.
Methods
The Nationwide Readmissions Database (2010–2022) was queried for patients with ACLF using previously validated algorithms admitted with variceal upper GI bleeding who received endoscopic intervention. Patients were stratified into two groups: therapeutic EGD with pTIPS and therapeutic EGD alone (band ligation). Primary outcomes were 30- and 90-day unplanned readmissions and readmissions for GI bleeding. Secondary outcomes included readmissions for intracranial hemorrhage (ICH) and blood transfusion. Multivariable hierarchical regression adjusted for demographics and comorbidities was performed, with statistical significance defined as p< 0.05.
Results
A total of 142,969 patients were identified, of whom 6,963 (4.6%) underwent pre-emptive TIPS in addition to EGD. These patients had a greater comorbidity burden (mean Elixhauser score: 19.3±7.2 vs. 17.2±7.1; p< 0.001). Predictors of pTIPS utilization are shown in Table 1. Compared with EGD alone, EGD plus pTIPS was associated with higher odds of unplanned readmission at 30 days (OR 1.29; p< 0.001) and similar odds at 90 days (OR 1.09; p=0.13). In contrast, patients who underwent EGD plus pTIPS had significantly lower odds of GI bleed-related readmission at 30 days (OR 0.55; p< 0.001) and 90 days (OR 0.46; p< 0.001). Secondary analyses showed reduced transfusion-related readmissions at 90 days (OR 0.71; p< 0.001) and similar odds at 30 days (OR:0.88; p=0.29).
Conclusion
In patients with ACLF presenting with variceal bleeding, therapeutic EGD combined with pTIPS (within 72 hours of index endoscopy) was associated with fewer GI bleed-related readmissions and lower transfusion requirements, but at the cost of higher 30-day unplanned readmission. These findings highlight the importance of early GI–IR collaboration in selecting ACLF patients who may derive the greatest benefit from the addition of pTIPS to standard endoscopic therapy. Incorporating additional clinical variables such as hepatic encephalopathy will be essential to refine selection criteria and optimize outcomes.
-

Post-Operative Afib After CABG: A Retrospective Analysis
Leonardo A. Almaguer Gongora, Myrna E. Reinhardt, Manuel Jimenez, Luis E. Remedios Carbonell, Daniel Padron, Priya Mohan, Juliette Camejo, and Bernardo Reyes
-

Life Over Limb: A Case of Rapidly Rrogressive Necrotizing Fasciitis
Olesya A. Balashova, Adam Lerchenfeld, Rahul Ramakrishnan, Ashley Diaz, Anna Felizcek, and Daniel Heller
-
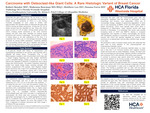
Carcinoma with Osteoclast-like Giant Cells: A Rare Histologic Variant of Breast Cancer
Robert Bender, Makenna Bowman, Matthew Lee, and Susana Ferra
Introduction: Osteoclast like giant cells (OGCs) can be found in various tissues such as the gallbladder, liver, pancreas, and thyroid. In breast cancer, the presence of OGCs is a rare finding. Currently knowledge of such cases is limited, with approximately 200 reported cases of osteoclast like giant cells (OGCs) among all breast carcinomas. Among the breast cancers that are classified as rare, those with OGCs make up only 0.5-1.2% of cases.
Case Description: An 80+ year-old female presented with a palpable left breast lesion initially suspected by mammography as a benign lesion. She eventually underwent breast core biopsy revealing hormone positive, Her2 negative invasive ductal carcinoma. A left breast mastectomy and sentinel lymph node (SLN) resection were performed.
Results: Pathology revealed a well circumscribed 3.8 cm rubbery hemorrhagic mass with cribriform morphology, numerous osteoclast-like multinucleated giant cells OGCs and hemosiderin-pigmented macrophages. No tumor was present in the SLN. A diagnosis of Invasive Carcinoma with OGCs Grade 1 was rendered.
Discussion: Osteoclast like giant cells are multinucleated giant cells with eosinophilic cytoplasm that are similar to osteoclasts in both morphology and function. Breast cancers with OGCs are typically invasive breast carcinoma of no special type. In contrast to previous reports where the average age of occurrence is around 45-46 years old, our case is an 80+ year old female. Approximately 50% of women with breast cancer with OGCs received a diagnosis of benign lesion on as it occurred in our case.
Conclusion: We present a case of a rare histologic variant of invasive breast cancer with osteoclast like giant cells. With relatively few cases published, we provide an additional case with morphologic and histologic descriptions of this unique type of breast cancer.
-
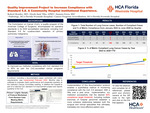
Quality Improvement Project to Increase Compliance with Standard 5.8: A Community Hospital Institutional Experience.
Robert Bender, Nicole Sant 'Elia, and Susana Ferra
Background: The Commission on Cancer (CoC) was established by the American College of Surgeons in 1922. In 2020, they launched the Cancer Surgery Standards Program that introduced six operative standards. Standard 5.8 requires curative intent lung resections to include sampling from at least 1 hilar, and at least 3 mediastinal lymph node stations.
Goal: To increase our institution’s compliance with CoC standard 5.8 to greater than 80% overall adherence.
Method: Included in the study were patients undergoing curative intent lung resection for lung cancer. A protocol, including a documentation paper worksheet with metric requirements, was implemented in February 2024. Monthly data was collected to evaluate metric performance and presented quarterly at our institution’s Cancer Committee meeting. The hospital is also part of a national CoC standard 5.8 improvement project and reports quarterly to the CoC.
Results: The percentage of compliant cases was 70.5% in 2023, and rose to 75% in 2024. So far in 2025, the compliance percentage has risen to 87.5%, successfully surpassing the 80 percent metric target compliance goal.
Conclusion: Implementation of this documentation protocol enables a quantitative method of monitoring compliance with the CoC 5.8 standard. With a little over a year since implementation, our institution successfully met the desired 80% compliance target threshold.
-

When Appendiceal Obstruction Looks Metallic: An Unusual Radiologic Presentation of Appendicitis
Nathan Cohen and Gary Padilla-Maldonado
Introduction: Right lower quadrant pain is a common presentation of acute appendicitis, but presentations in elderly patients may be subtle. Appendiceal obstruction is frequently caused by fecaliths; however, not all radiopaque findings in the appendix represent fecaliths. Rarely, these obstructions can mimic metallic foreign bodies on imaging, complicating interpretation and management. This case highlights an unusual radiologic presentation of appendiceal obstruction with metallic appearance, underscoring the importance of careful image analysis in atypical cases of appendicitis.
Case Description: An elderly man presented to the emergency department with a three-day history of constant right lower quadrant abdominal pain. He denied associated gastrointestinal or urinary symptoms. On arrival, vital signs demonstrated a mild fever (38.3-38.6 C) and elevated blood pressure (>160/102 mmHg). Physical examination revealed localized right lower quadrant tenderness with mild guarding and a positive McBurney’s point, without other significant findings.
Laboratory evaluation showed leukocytosis with a WBC count of 15.4x103 / µL and neutrophilia (84.4%). Coagulation panel was unremarkable. Chemistry panel revealed mild hyponatremia (Na 133 mmol/L) and elevated total bilirubin (1.4 mg/dL). Urinalysis was notable for ketonuria and red blood cells, but without pyuria or leukocyte esterase.
CT of the abdomen and pelvis demonstrated a distended appendix with wall enhancement, peri-appendiceal fat stranding, and a radiopaque focus at the appendiceal ostium, initially concerning for a metallic foreign body. Abdominal X-ray confirmed a high-density object in the right lower quadrant.
Surgical consultation led to laparoscopic appendectomy. Intraoperative findings revealed a gangrenous appendix with localized peritonitis. The procedure was completed with minimal blood loss and no complications. The patient’s postoperative course was uncomplicated, with normalization of vital signs under hospitalist co-management with IV antibiotics and pain control.
Pathology confirmed acute perforated gangrenous appendicitis with severe peri appendiceal acute inflammation. The radiopaque object visualized on imaging was discarded intraoperatively and not included in the specimen submitted for pathological evaluation.
Discussion: The decision to proceed with surgical intervention was based on the patient’s clinical presentation, laboratory findings, and imaging studies. The persistent right lower quadrant pain, fever, and leukocytosis were consistent with acute appendicitis, while imaging demonstrated a radiopaque focus at the appendiceal base. Although the appearance initially raised suspicion for a metallic foreign body, the possibility of an obstructing fecalith was strongly considered, as both can present with high-density artifacts on CT and X-ray. Given the risk of perforation and peritonitis associated with fecalith-related appendicitis, prompt laparoscopic appendectomy was recommended.
This case highlights an important radiological pitfall: radiopaque appendiceal obstructions can mimic metallic foreign bodies, potentially leading to diagnostic confusion. Awareness of this overlap is essential, as misinterpretation could delay appropriate surgical consultation. Another important lesson is the value of specimen preservation for radiology-pathology correlation, as discarding the radiopaque object prevented definitive identification in this case. Ultimately, clinicians must integrate imaging findings with clinical context when evaluating appendicitis, particularly in elderly patients with atypical or subtle presentations. Early recognition and surgical management remain key to preventing complications such as gangrene or peritonitis.
-

Comparing ChatGPT and DeepSeek for Deprescription Support in Geriatric and Palliative Care: An Exploratory Study Using Clinical Vignettes
Gokhan Demir, Angel Sanchez, and Sanaz Kashan
Background: Polypharmacy is common in older adults and increases risks of adverse drug events, falls, and hospitalizations. Deprescription can mitigate these harms but is often hindered by time constraints, fragmented guidelines, and complex comorbidities. Artificial intelligence (AI) large language models (LLMs) may provide decision-support for deprescription in geriatric and palliative care.
Objective: To compare ChatGPT and DeepSeek in their deprescription recommendations across standardized polypharmacy vignettes.
Methods: Three validated clinical vignettes, varied by activities of daily living (ADL) status and cardiovascular disease (CVD) history, were presented to ChatGPT (GPT-4/5) and DeepSeek (2024 version). Each vignette was tested in three replicates per model. Outputs were analyzed for (1) binary deprescription decisions, (2) medications targeted, and (3) replicate consistency. Results: In patients without CVD, both models consistently recommended deprescription across all ADL scenarios. In patients with CVD, ChatGPT was more variable (e.g., deprescription rates ranged from 0–67% across replicates), whereas DeepSeek consistently recommended deprescription in 100% of scenarios. Both models most often targeted gastrointestinal and pain medications. ChatGPT demonstrated high replicate stability in the no-CVD scenarios, while DeepSeek showed complete stability across all scenarios.
Conclusion: Both ChatGPT and DeepSeek show promise as adjuncts for deprescription decision-support in geriatrics. DeepSeek demonstrated greater conservatism in CVD cases but higher internal consistency, whereas ChatGPT was more aggressive but variable. LLMs may augment deprescription reviews but require expert oversight and validation against established frameworks.
-

Acute Respiratory Compromise Secondary to Superior Vena Cava Syndrome in a Sickle Cell Patient. Vaso-occlusion triggered by Steroids?
Ashley Diaz, Priya Mohan, Abhishek Sharma, David Zarabanda, and Raiko Diaz
-
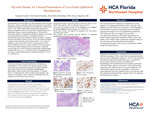
Myxoid Variant: An Unusual Presentation of Low-Grade Epithelioid Mesothelioma
Racquel Fournet, Robert Bender, Rohit Jaishankar, and Alexey Glazyrin
-

Distinguishing Narcolepsy Hallucinations From Drug-Induced Hallucinations In An Adolescent With Comorbidities
Avidor Gerstenfeld, Biwy Emmanuella Cadet, Salma Alkhatib, and Annette Santiago
-

The Role of Bandemia in Clinical Outcomes of Critically Ill Septic Patients.
Yerandi Gil, Grettel Gonzalez Garcia, Ambar Sekulis, Rafael Miret, Siddarth Kathuria, Mauricio Danckers, and Daniel Heller
Rationale: Bandemia, defined as the presence of immature neutrophils in circulation, is commonly used as an early marker of systemic inflammation and infection. 1 However, its prognostic significance in sepsis, severe sepsis, and septic shock remains uncertain. 1-2 This study aimed to determine whether bandemia is associated with adverse clinical outcomes and increased intensive care unit (ICU) resource utilization among critically ill septic patients admitted from the emergency department (ED).
Methods: A retrospective analysis was conducted using de-identified data from the HCA Healthcare database. Adult patients (aged 18–90 years) admitted to the ICU at HCA Florida Aventura Hospital from the ED between May 1 and June 30, 2024, with a diagnosis of sepsis, severe sepsis, or septic shock were included. Sepsis-related diagnoses were identified using contemporary ICD-10 criteria consistent with the Sepsis-3 era.3 Exclusion criteria were absence of differential band count and comorbidities that could confound bandemia (e.g., hematologic malignancy, systemic lupus erythematosus, human immunodeficiency virus infection, recent chemotherapy, or corticosteroid use). Patients were categorized by bandemia level: < 10% vs ≥10%. 4 Primary outcomes were all-cause in-hospital mortality and ICU length of stay (LOS); secondary outcomes included vasopressor and invasive mechanical ventilation use. Statistical analyses included t-tests and chi-square tests as appropriate, and regression analysis to identify factors associated with bandemia.
Results: Of 9,115 encounters identified, 1,315 patients met inclusion criteria, of which 41.2% had bandemia ≥10%. In-hospital mortality was slightly higher among patients with bandemia compared to those without (22.5% vs 21.0%), but the difference was not statistically significant (p=0.5198). 5 The mean ICU LOS was similar between groups (9.10 vs 9.12 days, p=0.395). [Table 1] Use of vasopressors and mechanical ventilation was more frequent among patients with bandemia (72.7% and 49.7%, respectively) compared with those without bandemia (64.3% and 42.0%). Regression analysis identified age as the only variable significantly associated with bandemia, with each additional year of age corresponding to a 0.76% increase in the odds of bandemia (p=0.0347).
Conclusions: Although bandemia was associated with increased utilization of ICU interventions, it was not independently predictive of mortality or ICU length of stay in critically ill septic patients. These findings suggest that while bandemia may reflect underlying illness severity, it has limited value as a standalone prognostic marker in sepsis
-

Cocaine Induced Agranulocytosis and Neutropenia
Maria Gomez Alvarez, Ashish Govan, and Raymond LaRocque
Introduction: Cocaine use in the United states is seen in many cases within the hospital system. Typically, they present with tachycardia, hypertension, sweating, even heart attack. Due to the uncontrolled sale and distribution of drugs, patients can be exposed to other additives in drugs which can lead to unexpected complications. Cocaine laced with levamisole (an antiparasitic drug used in veterinary medicine) can lead to agranulocytosis and neutropenia. Cocaine being the second most used illegal drug following marijuana it may be much more common than we think. Millions of individuals use cocaine yearly and develop a heavy addiction with use of other drugs as well. These undetectable combinations can be life-threatening and misleading in treatments and procedures that patients undergo within the hospital system.
Case Description: The patient is a 60-year-old male who presented to the facility complaining of abdominal pain. He previously had visited the facility several days prior and was discharged and diagnosed with constipation. He continued to have abdominal pain and constipation. The patient was found to have WBC count of less than 1. A drug screen was positive for cocaine use. As the patient improved with fluids, and a bowel regimen the patient continued to have undetectable WBC level and eventually became neutropenic with a fever. The patient was placed on appropriate precautions and antibiotics and recovered.
The patient remained in the hospital setting for additional testing and continued to come back negative for sexually transmitted illnesses and bone marrow biopsy was negative for any infiltration or pathology. After extensive discussion regarding his medical history, the patient discussed with both the primary and hematology team that he was a long-term cocaine user and had different sources for obtaining the drug. After more than a week in the hospital the patient’s WBC count began to rise within normal reference range. The patient recovered and was counseled extensively and had great family support within and out of the hospital.
Discussion: The patient’s case demonstrates and importance of understanding that typical drug use does not present in the manner which we may be accustomed. It is important for clinicians to understand and recognize that patients consume drugs that may be laced with other drugs that are not commonly seen within the hospital setting and that the side effects can be life-threatening in ways for which are not expected. A thorough discussion on patient drug use can be very uncomfortable and awkward at times but it proves to be essential in understanding what is happening to patients, how to diagnose, treat, and avoid unnecessary tests for the patient. This also provides tools for physicians to use as counseling for drug cessation
-
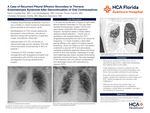
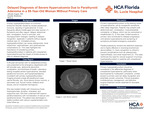
A Case of Recurrent Pleural Effusion Secondary to Thoracic Endometriosis Syndrome After Discontinuation of Oral Contraceptives
Kevin Gopala-Rao, Luis Santiesteban, Carmen Tormo Carrillo, Christian Almanzar Zorilla, and Mauricio Danckers
Introduction: Thoracic endometriosis syndrome (TES) is a rare condition in which functional endometrial tissue spreads to the thoracic cavity. Manifestations of TES include catamenial hemoptysis, pneumothorax, and pleural effusions along with symptoms of dyspnea, cough, and pleuritic chest pain.1 Approximately 6 to 10% of women of reproductive-age women develop TES with concurrent pelvic endometriosis in 80% of patients.2 Treatment of TES includes medical management with progesterone-based oral contraceptive pills (OCPs) and surgical management involving cardiothoracic surgery. We present a case of recurrent pleural effusions in a patient who was non-compliant with medical management of TES. Methods: Data was collected during this admission. Case Description: Patient is a 35-year-old female with a history of uterine fibroids, right-sided pleural effusion secondary to TES, presented with a dry cough and progressive dyspnea. Duration of symptoms lasted for 2 weeks before seeking medical attention from her established pulmonologist and cardiothoracic surgeon. About 1 month prior to onset of symptoms, she stopped taking daily OCP, progesterone-drospirenone, due to her desire for pregnancy. MRI chest revealed a right-sided pleural effusion with regions of nodular pleural thickening, in addition to a new right hemi-diaphragmatic lesion. In 2018, she had a similar presentation in addition to pleuritic chest pain that radiated to the right subscapular region with similar findings on CT chest at that time. The patient underwent a video-assisted thoracoscopic surgery (VATS) and pleurodesis with a cytology revealing endothelial glandular tissue and blood. Given her history of TES, the patient underwent a second VATS and pleurodesis with similar cytology results from the pleural fluid. Pathology of the right hemi-diaphragmatic lesion revealed endometrial glandular and stromal tissue. She was managed post-operatively for 1 week and discharged home with instructions to resume OCPs. Discussion: Extra-pelvic endometriosis may occur in different areas of the body, including the thoracic cavity, gastrointestinal tract, and urinary tract. The pathophysiology of TES is based upon Sampson’s theory of retrograde menstruation, in which endometrial cells travel from the fallopian tubes into the peritoneal cavity to the right paracolic gutter and travel to the pleural cavity via transperitoneal-transdiaphragmatic migration from either acquired fenestrations in the diaphragm or congenital anomaly. 1 Without progesterone-based OCPs, migrated endometrial tissue will proliferate and result in breakthrough bleeding, leading to accumulation of fluid in the thoracic cavity. Conclusion: Although the incidence of TES is approximately 6 to 10% of reproductive-age women, researchers hypothesize that the incidence rate is much higher. This is mainly due to underdiagnosis and under-reporting cases in general. Unfortunately, underdiagnosis is common in patients with TES, given that the risk factors and clinical presentation may mimic more prevalent conditions in pulmonology and gynecology. Even with recent advancements in medicine and surgery, studies have reported recurrence rates of 14.3 to 55%, making management and symptom relief challenging.3 While the recurrence rate remains high, it is imperative to educate patients on medication compliance, routine follow-up with respective specialties, and signs and symptoms of recurrence. Bringing awareness of risk factors and clinical presentation can assist clinicians in making an early diagnosis of TES.
-

Comparing Efficacy of Psychotropic Classes to Control Aggression Among Pediatric Patients Hospitalized with Oppositional Defiant Disorder
Orestes Hadjistamoulou, Sindhura Kompella, Melissa Ricardo, and Samuel Neuhut
-

Avatrombopag-Induced Thrombocytosis Leading to Pulmonary Embolism in a Patient with Refractory ITP
Rohit Jaishankar, Kristine Peligrino, Alejandra Rinaldi, and Racquel Fournet
-
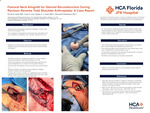
Femoral Neck Allograft for Glenoid Reconstruction During Revision Reverse Total Shoulder Arthroplasty: A Case Report
Devin Q. John, Leon Z. Liu, Diego J L Lima, and Howard D. Routman
-

Lactate/Albumin and RDW/Albumin Ratios for Mortality and Readmission in Post-MI Heart Failure
Amogh Killedar, Hamza Khan, and Henry Cusnir
BACKGROUND Robust biomarkers that capture the combined effects of inflammation and tissue hypoperfusion, are needed to refine post–acute myocardial infarction (AMI) risk stratification—especially in the large subset that develops congestive heart failure (CHF). Two emerging candidates are the lactate/albumin ratio (LAR) and the red-cell-distribution-width/albumin ratio (RAR). Separate studies have linked each ratio to short- and long-term mortality in critical illness, AMI, and heart failure, yet no work has directly compared their performance together. We addressed this evidence gap in a large, multi-hospital dataset.
METHODS We performed a retrospective analysis of 8 115 encounters drawn from the HCA Healthcare database (2016-2024). Adults with confirmed AMI complicated by CHF and documented lactate, RDW, and albumin levels were included; those lacking labs and relevant data were excluded. Primary outcome was all cause mortality at index encounter, with secondary being 7,15 & 30-day readmissions. Predictors entered into logistic regression were descriptives, LAR, RAR, and PCI status. Model discrimination was assessed with the concordance statistic. We chose our LAR and RAR cutoff values as 0.5 and 4.65 respectively from previous studies.
RESULTS Elevated LAR and RAR each independently increased the odds of death after adjustment for demographics and PCI. For LAR, the odds of mortality were nearly tripled (OR 2.99, 95 % CI 2.62–3.42; p < 0.001). RAR exerted a significant, but comparatively smaller association, (OR 1.68, 95 % CI 1.50–1.89; p < 0.001). Female sex, non-White race, and receipt of PCI were protective (all p < 0.05). The full model achieved moderate discrimination (C = 0.708). Importantly, elevated LAR, but not RAR, predicted early clinical deterioration, being significantly associated with 7, 15 and 30-day readmissions.
CONCLUSION Both LAR more than RAR are powerful, readily obtainable predictors of short-term mortality in CHF patients recovering from AMI, with LAR also signaling readmission risk. Routine calculation of these ratios at admission could sharpen bedside prognostication & prompt increased surveillance. Incorporating ratios into post-AMI care warrants prospective validation and may foster a habit of leveraging routinely collected laboratory data for precision cardiac medicine.
Elevated LAR at index admission contrastingly was significantly associated with reduced with 7,15,30-day readmissions by 13-19% , possibly suggesting worse clinical presentations at index admission leading to prompt PCI. This, however, should be independently further evaluated through a much larger study for higher power by increasing the sample size. Interestingly, PCI at index encounter also had high association with 7-day readmissions, suggesting the need of detailed vigilance through clinical modalities prior to discharges.
-

CD10 Positive Mantle Cell Lymphoma Masquerading as Follicular Lymphoma
Matthew Lee, Jennifer Barker, and Fatemeh Mousavi
-
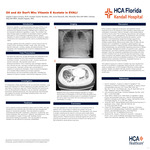
Oil and Air Don’t Mix: Vitamin E Acetate in EVALI
Angelo Lopez-Lacayo, Jordan Taylor-Bentley, Josef Masseli, Michelle Silva, Christy Diaz, and Daniel Zapata
Introduction: Electronic cigarette or vaping-associated lung injury (EVALI) is an acute or subacute condition characterized by acute respiratory symptoms and bilateral pulmonary infiltrates seen in patients who are exposed to electronic cigarettes or vapes. The condition has been strongly linked to inhalation of aerosolized vitamin E acetate, particularly in THC-containing e-cigarette products. Despite regulation of vitamin E acetate in the production of electronic vapes, it continues to be a byproduct of EVALI due to counterfeit electronic vapes. Clinically, patients with EVALI present in various ways but are not limited to fever, shortness of breath, cough, chills, body aches, pleuritic chest pain, vomiting, nausea, and abdominal pain. Prompt recognition and management are crucial for mitigating adverse outcomes. Case Presentation: We report the case of an 18-year-old female who presented to the emergency department with initial complaints of progressive shortness of breath, nonproductive cough, vomiting, nausea and pleuritic chest pain. She reported recent use of tetrahydrocannabinol (THC) containing vape cartridges obtained from informal sources. Vital signs revealed tachycardia, tachypnea, and hypoxemia. Laboratory studies were unremarkable for infectious or autoimmune etiologies. Chest computed tomography (CT) revealed diffuse bilateral ground-glass opacities. Bronchoscopy with bronchoalveolar lavage (BAL) identified the presence of vitamin E acetate, confirming the diagnosis of EVALI. Investigations CT angiography initially performed to rule out pulmonary embolism. Lung fields were significant for diffuse bilateral ground-glass opacities with 5-year history of electronic vape use. Further infectious and autoimmune work up was performed to attempt to rule out vasculitis, eosinophilic pneumonia, bacterial pneumonia, and viral pneumonia. Bronchoscopy was negative for alveolar hemorrhage indicating further work up for possible vitamin E exposure. Treatment Due to patients worsening respiratory status while on HFNC, she was transferred to the intensive care unit where she was intubated and placed on mechanical ventilation. She was started on systemic corticosteroids 60mg BID, levalbuterol, ipratropium, budesonide, and empiric antibiotics with vancomycin, cefepime, and azithromycin. She was intubated for roughly 72 hours with moderate clinical improvement leading to extubation. She was educated on smoking cessation as well referred for pulmonary rehabilitation. Discussion: EVALI remains a diagnosis of exclusion with significant clinical implications due to its potential for rapid respiratory deterioration and multisystem involvement. Vitamin E acetate, a lipid-soluble additive commonly found in illicit THC-containing vape products, has emerged as a key agent in EVALI pathogenesis. Its interference with pulmonary surfactant leads to a chemical pneumonitis-like reaction, and its detection in bronchoalveolar lavage fluid strongly supports the diagnosis when aligned with clinical and radiologic findings. The condition predominantly affects young males under 35 years old and presents with a constellation of respiratory, gastrointestinal, and constitutional symptoms. Imaging typically reveals bilateral infiltrates, while histopathology may demonstrate organizing pneumonia or diffuse alveolar damage. Management centers on supportive care, systemic corticosteroids, and empiric antibiotics pending exclusion of infectious etiologies. Given the nonspecific presentation and overlap with more common conditions such as community-acquired pneumonia, a high index of suspicion and detailed vaping history are critical. Public health measures should continue to emphasize avoidance of THC-containing vaping products, particularly those from unregulated sources, to prevent recurrence and reduce morbidity. This patient’s exposure to vitamin E acetate may have resulted from the use of counterfeit or unregulated vaping products, which were widely circulated prior to FDA oversight of electronic nicotine delivery systems. Notably, the patient had easy access to these products through a family connection, as their father was employed/owner of a smoke shop. Conclusion: This case highlights the critical importance of considering EVALI in patients with a recent history of vaping who present with acute respiratory and gastrointestinal symptoms. The association with vitamin E acetate underscores the need for continued public health efforts, regulatory oversight, and education regarding the risks of unregulated vaping products. Patients should be cautioned against the use of such products and advised to avoid all forms of tobacco and vaping due to their potential to cause serious lung injury.
-
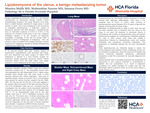
Lipoleiomyoma of the Uterus, a Benign Metastasizing Tumor
Munira Malik, Mohtashim Naeem, and Susana Ferra
-

Advantages of Humeral Stem Retention in Revision Shoulder Arthroplasty: A Retrospective Study
Matthew McCrosson, Leon Liu, Daniel DeShetler, John Grossi, Devin John, Diego Lima, and Howard Routman
-
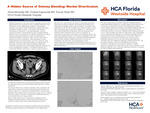
A Hidden Source of Ostomy Bleeding: Meckel Diverticulum
Shiva Morisetty, Ezekiel Kapusiak, and Kumar Shah
Adult Meckel diverticulum can present atypically compared to classic childhood Meckel diverticulum. Given the increased likelihood of concurrent medical conditions in adults, it is often overlooked in the differential for lower gastrointestinal bleeding. We report a 61-year-old male with rectal adenocarcinoma status post low anterior resection and diverting loop ileostomy who presented repeatedly with hematochezia via the ostomy. Prior episodes were managed conservatively. During the index admission, esophagogastroduodenoscopy and ileoscopy did not identify a bleeding source; a clip was placed near the suspected site. Interventional radiology was consulted for mesenteric angiography. Superior mesenteric angiography demonstrated a tortuous aberrant ileal branch extending beyond the vasa recta arcade with a focal vascular blush in the right lower quadrant—findings suspicious for a persistent omphalomesenteric (vitelline) artery supplying a Meckel diverticulum. Selective embolization of the culprit branch achieved immediate hemostasis, with resolution of bleeding and an uncomplicated recovery. A post-embolization Tc-99m pertechnetate scan subsequently confirmed Meckel diverticulum. This case highlights that, in adults with lower gastrointestinal bleeding of unclear etiology—including bleeding through an ileostomy—Meckel diverticulum remains an important, albeit uncommon, consideration. Targeted angiography by interventional radiology can both control hemorrhage and suggest the diagnosis.
-

Turmeric, Red Yeast Paste, and Statins: A recipe for DILI
John V. Nahas, Sinay Ceballos, and Franklin Kasmin
Introduction Drug induced liver injury (DILI) contributes to a significant portion of acute liver injuries and acute liver failure in the west. DILI accounts for approximately 11% of acute liver failure cases in the US according to ACG. Insulting agents are numerous and well documented in the NIH LiverTox database, however the rarity and complexity of individual agents is a matter of ongoing study. Case Description/Methods A 52 year old man with PMH of HTN and HLD presents for a 2 week history of abdominal swelling, bilateral lower extremity swelling, decreased appetite, and positional shortness of breath. He endorses occasionally drinking an oz. of vodka before bed to fall asleep but denied heavy binge drinking. His medications were amlodipine, HCTZ, and atorvastatin. Of note this patient was very health conscious and took a regimen of natural remedies including turmeric pills, red yeast paste, Zinc, and fish oil. Labs were significant for ALT = 815 u/L, AST = 2480 u/L, Alk Phos = 238 u/L, T. Bilirubin = 3.2 mg/dL and creatinine phosphokinase (CPK) = 18,000 u/L. An infectious workup was negative for viral hepatitis, syphilis, and Leptospira. Immunological workup was negative for ANA, Anti-smooth muscle ab, and Anti-LKM ab. An abdominal US revealed trace subhepatic ascites. Portal vein US showed patent hepatopetal flow. CT scan showed a normal size and contour of the liver. An echocardiogram showed normal left ventricle with 55% ejection fraction. After home medications were discontinued, the liver function tests and CPK trended down. Spironolactone helped reduce swelling. Discussion This is a case of new onset hepatocellular pattern (R factor 7.4) acute liver injury without past chronic hepatic disease. DILI second to atorvastatin, turmeric, and Red Yeast use was the presumed diagnosis as these agents have likelihood scores of A, B, and C respectively. Although statins are a class A cause of liver injury, the incidence of a >3x elevation of ULN is exceedingly rare (< 1% of cases) In the case of turmeric induced DILI, most cases present with mild elevations of Alk. Phos. and marked elevation of AST and ALT ( > 1000). Interestingly most reports of turmeric induced DILI had a combination of multiple offending agents such as this case. Red yeast is a traditional Chinese herbal remedy containing monacolin K, an identical agent to lovastatin. Prospective controlled studies do not show a significant enzyme increase in LFTs, but there are isolated case reports with liver injury second to consumption of red yeast.
-

Emerging Role of Liafensine in the Treatment of Treatment Resistant Depression: Insights from the Enlighten Trial
Karla Narvaez, Saad Masud, and Richard Callahan
Background: Treatment-resistant depression (TRD) remains a significant unmet need, affecting about one third of patients with major depressive disorder who fail to respond to two or more antidepressant trials. There is a need for new pharmacological approaches. Liafensine (also known as DB104) is a first-in-class triple reuptake inhibitor targeting serotonin, norepinephrine, and dopamine transporters, whose development has recently incorporated a precision medicine approach. Mechanism of Action: Liafensine inhibits reuptake of all three major monoamines (serotonin, norepinephrine, and dopamine) distinguishing it from existing SSRIs, SNRIs, or other agents which typically target one or two systems. A genetic biomarker, ANK3 (also called DGM4), has been identified as predictive of treatment response. Approximately 20% of TRD patients carry the ANK3-positive genotype, which appears to correlate with improved efficacy in clinical trials. Clinical Evidence: -Phase 2b ENLIGHTEN trial → enrolled 189 ANK3-positive treatment-resistant depression patients. Patients were then randomized to receive either: liafensine 1 mg, liafensine 2 mg, or placebo daily, over 6 weeks. -The primary outcome (change in the Montgomery-Åsberg Depression Rating Scale (MADRS) from baseline to week 6), → revealed a mean reduction of −15.4 in liafensine-treated patients vs −11.0 in placebo, resulting in a mean treatment difference of −4.4 points (95% CI, −7.6 to −1.3; p = .006). -Secondary outcomes (Clinical Global Impression-Severity, Clinical Global Impression-Improvement, Sheehan Disability Scale) were also positive for liafensine. Patients began to improve during the first week. -Research shows ideal dosing is low: both 1 mg and 2 mg daily showed similar efficacy, with better tolerability at 1 mg. -Limitations: relatively short trial duration (6 weeks), limited long-term data, and the fact that efficacy was only demonstrated in the ANK3-positive subgroup (populations without this biomarker in earlier trials did not show benefit). Conclusion: Research shows liafensine is a new drug therapy for treatment resistant depression when applied in a biomarker-guided fashion. The ENLIGHTEN trial shows clinically meaningful benefits with good safety in ANK3‐positive patients. Further longer-term trials and studies in diverse populations are needed to establish its place in practice.
-

Closing the Communication Gap: A Quality Improvement Approach to Safer Shift Changes and Transfers
Stephanie O'Kresik Jewette and Annette Santiago
-

Platypnea-orthodeoxia Syndrome in a Case of Septal Occlusion Device Migration
Bike Ozkan, Richard Shalmiyev, Adam Devine, Michael Pelekhach, Siddarth Kathuria, Daniel Heller, and Mauricio Danckers
Introduction
Platypnea-orthodeoxia syndrome (POS) is defined by dyspnea and hypoxemia in the upright position, which improves upon recumbency. While often linked with hepatopulmonary syndrome, intracardiac etiologies, particularly a patent foramen ovale (PFO), may also be responsible. PFOs are typically managed with device closure, and while rare, device migration can occur unbeknownst to the patient with resultant critical sequelae.
Methods
Here, we present the case of an 89-year-old female with a medical history of hypertension, diabetes, and coronary artery disease status post PCI, who arrived with severe dyspnea and was subsequently intubated for profound hypoxia. A chest CT angiogram ruled out pulmonary embolism but identified a foreign object in the pulmonary artery. A bubble contrast echocardiogram confirmed a septal defect and PFO. Further patient history revealed prior placement of a PFO closure device in her native country 30 years ago. Following extubation, she was found to remain significantly hypoxic when sitting and required high-flow nasal cannula support whenever upright, consistent with POS. Her work-up remains ongoing.
Results
POS results from right-to-left shunting of blood, bypassing pulmonary oxygenation. This can occur through intracardiac or intrapulmonary shunts. In this case, migration of the septal closure device likely re-established an interatrial communication, permitting right-to-left shunting and POS physiology due to elevated right atrial pressures.
Conclusions
Our case highlights the importance of considering prior device-related interventions in patients with unexplained hypoxemia and evaluating oxygenation changes in different body positions for added diagnostic value.
-

Severe Hypersensitivity Reaction After Unsupervised Hyaluronic Acid Filler Injection
Kevin Posner and Julia Fashner
-

Real Time Non-targeted Renal Biopsy Adequacy Evaluation: A Successful Quality Improvement Activity
Astrid Sacasa and Susana Ferra
Introduction. Adequate renal biopsies are essential for the diagnosis and treatment of medical renal disease. This process requires a sufficient number of glomeruli for light microscopy, immunofluorescence, and electron microscopy evaluation. On-site microscopic evaluation of kidney biopsy specimens significantly improves sample adequacy and the ability to render a diagnosis, with studies showing a much higher rate of inadequate samples when on-site evaluation is absent. Inadequate biopsies can have a significant negative impact on patient care including delay of adequate diagnoses, worsening of the patients’ condition and complications, and increasing costs due to the need for repeat biopsies. A real time on-site evaluation of kidney biopsies adequacy protocol was introduced in our institution on April 2019.
Methods. The goal was to document improved adequacy of non-targeted kidney biopsies after protocol implementation using a dissecting microscope and a protocol for on-site adequacy evaluation introduced on April 2019. Annual inadequacy rates were calculated, using a two-proportions calculation with α 0.15 and Fisher exact test to determine the statistical significance between data from 2017 and 2018, and 2023 and 2024.
Results and conclusion. The results showed a decrease in the inadequate biopsy rates from 23- 25% to 8.3-5% after implementation of the on-site quality improvement protocol, with return of investment after the first case, considering the cost of a repeat biopsy. In addition, we establish a more cohesive relationship between nephrology, interventional radiology and pathology with a significant increase in physician satisfaction that ultimately translates into more effective patient care.
-

Primary Cardiac Lymphoma: A Rare Diagnosis
Astrid Sacasa, Betty Kirimi, Mohtashim Naeem, and Susana Ferra
-

Performance in Grading of Well Differentiated Pancreatic Neuroendocrine Tumors (WDPanNET) Using the 2019 World Health Organization (WHO) Classification of Tumors of the Digestive System. Experience of a Community Teaching Hospital.
Astrid Sacasa, Gul Emek Wymer, and Susana Ferra
CONTEXT: The WHO Classification of Tumors of the Digestive System (2019) categorizes WDPanNETs as grade 1 (G1), grade 2 (G2) or grade 3 (G3) by mitotic count and proliferative index (KI67). We examined the performance of pathologists and pathology trainees in grading WDPanNET according to the 2019 WHO Classification.
DESIGN: One H&E and KI-67 slides of eleven WDPanNET cases from our 2023 archives (7 G1, 1 G2 and 3 G3) were blindly evaluated by 2 junior residents (PGY-1), 2 senior residents (PGY-3), 2 pathologists without formal gastrointestinal training (NOGIP) and 2 pathologists with formal gastrointestinal training (GIP), provided with the 2019 WHO Classification. Their grading was compared with the reported grade of the case. Interrater agreement, accuracy and concordance by level of training were calculated.
RESULTS: The group interrater reliability was weak to moderate (ĸ = 0.488; z = 0.0189; p-value 0.985). Overall accuracy was 72.7%. By level of training, accuracy and (concordance) were 72.73% (81.82%) GIP, 81.82% (63.64%) NOGIP, 77.27% (72.73%) PGY-3 and 59.1% (54.55%) PGY-1. Only 2 cases (G1) were correctly classified by all participants. Grade accuracy was G3 (79.16%), G1 (71.42 %) and G2 (62.5%). Grade concordance was lowest (33.33%) for G3 by NOGIP followed by 42.86% for G1 by PGY-1. For G2 and G3, KI-67 was the determinant factor in all but one event. Eyeballing was the predominant method for KI-67 scoring.
CONCLUSIONS: Agreement was weak or at best moderate irrespective of level of training. There was remarkable variability in the KI-67 score among participants.
-

Perceptions of Presyncope versus Syncope: A Comparative Survey of Emergency Medicine and Hospitalist Providers
Jaime Said and Dennis Cardriche
-

Variability in Emergency Medicine Provider Practices for Recommending Days Off from Work or School by Chief Complaint
Jaime Said and Dennis Cardriche
-

Comparison of Diagnostic Accuracy of CT and SPECT-CT in Pseudarthrosis Detection: A Systematic Review and Meta-Analysis
Nicholas Schiller, Miguel Cartagena-Reyes, Elyette Lugo, Diego Lopes de Lima, Brett Schlifka, and Milad Alam
-
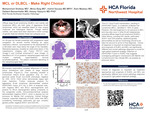
MCL or DLBCL - Make Right Choice!
Mohammed Shafeay, Mirza Baig, Astrid Sacasa, Ram Madasu, Delbert Benzenhafer, and Alexey Glazyrin
-

Investigating Secondary Causes of Hypertensive Emergency in a 37- year-old Adult with Multi Organ Involvement
Pallavi Shekhawat and Julia Fashner
-
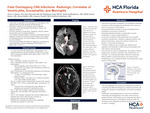
Fatal Overlapping CNS Infections: Radiologic Correlates of Ventriculitis, Encephalitis, and Meningitis
Jesse F. Simon, Sara Darwish, Stephanie Nagy, Richard Shalmiyev, David Kosoy, Bryan Rubio, Gustavo Pantol, and Mauricio Danckers
Introduction: This case study explores an uncommon triad of encephalitis, ventriculitis, and meningitis complicated by ischemic strokes and seizures in a COVID-19-positive patient. Prior studies suggest that bacterial meningitis and encephalitis can lead to cerebral infarctions due to inflammation and vascular injury.1,2,5 Ventriculitis, in particular, is rarely observed and typically is seen as a severe complication of meningitis, and can be managed with neurosurgical interventions such as CSF shunt placement, ventricular drains, or other intracranial devices.3,4 The simultaneous presentation of all three conditions in a single patient is rare and poses significant challenges from a diagnostic and management standpoint.
Case Presentation: We present a 73-year-old male with a history of hypertension, hyperlipidemia, and alcohol use disorder who was airlifted from a cruise ship for acute encephalopathy and respiratory distress from COVID-19. On arrival, treatment was initiated for alcohol withdrawal and community acquired pneumonia. At that time, he was septic with leukocytosis, hypertensive with an SBP > 200 mmHg, and initial head CT was negative for any acute abnormality. Several days later, a stroke alert was called for sustained left-sided weakness and worsening encephalopathy, prompting transfer to the ICU and intubation for airway protection. A lumbar puncture revealed findings suggestive of meningitis with purulent CSF and an opening pressure of 24 mmHg prompting immediate escalation of antibiotics. His MRI Brain revealed simultaneous ventriculitis, meningitis, and encephalitis. A repeat CT brain days later revealed ischemic infarcts in the right middle and anterior cerebral artery territories. Following progressive neurologic decline and no improvement over the next week, his spouse opted to transition him for hospice and palliative extubation.
Deviation from the Expected: The patient’s initial neurological state was attributed to alcohol withdrawal. Later CSF analysis and imaging revealed an uncommon infectious triad with significant infarcts.
Conclusion: The simultaneous presence of meningitis, encephalitis, and ventriculitis with stroke is infrequent, emphasizing the significance of broad differentials and importance of implementing comprehensive management strategies.
-

What Newly Updated Variables Are Correlated with Colon Cancer Incidence and Death Rates in Florida?
Cody Steed and Julia Fashner
-
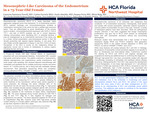
Mesonephric-Like Carcinoma of the Endometrium in a 73-Year-Old Female
Cameron Summers-Powell, Carina Ferraris, Zoyla Almeida, Susana Ferra, and Mirza Baig
Introduction: Mesonephric-like carcinoma (MLC) is a newly described malignant tumor that represents 1% of endometrial cancers. The etiology of this disease is currently unknown but immunohistochemical expression with GATA-3, PAX-8 and TTF-1 and lack of ER/PR positivity can aid in correct diagnosis.
Case Summary: A 73-year-old female presented to the hospital with post-menopausal bleeding, an initial hysteroscopy identified a lesion suggestive of endometrial cancer. Ultimately, the patient underwent a hysterectomy and a bilateral salpingectomy/oophorectomy. Chemotherapy ensued due to metastatic disease. At 7 months post-op, the patient appeared to be doing well.
Results: Grossly, the lesion was 5.5 cm and appeared to infiltrate the entire thickness of the myometrium. Microscopically, densely packed malignant glands were seen with eosinophilic secretions. GATA-3, PAX-8 and TTF-1 immunostains were all positive. ER and PR immunostains were negative. Finally, a wild-type staining pattern was seen with p-53.
Discussion: PIK3CA and KRAS mutations have been observed in other cases of MLC. Currently no standardized treatment regimen exists for this cancer; chemotherapy utilization including carboplatin and paclitaxel treatments are seen in medical literature. Researchers have explored the expression of the L1CAM adhesion molecule and have found higher expression in MLC compared to endometrioid endometrial carcinoma (EEC). Conclusion: Awareness of this entity is important due to its rarity, clinical course, and histological similarities to EEC. Ultimately, eosinophilic secretions on histology and the specific immunophenotype can help guide a diagnosis of MLC
-
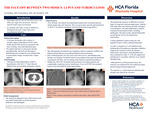
The Face-Off Between Two Mimics: Lupus and Tuberculosis
Fnu Swatisikta, Nang Kham, and Ali Chaudhry
INTRODUCTION Both lupus and Mycobacterium tuberculosis can affect any organ and can present with non-specific multi-organ involvement. In a patient with lupus, it may be difficult to distinguish between a lupus flare and a mycobacterial infection.
CASE A 28-year-old female with a history of systemic lupus erythematosus (SLE), (anti-Smith and ds-DNA positive), presented with knee swelling, chest and abdominal pain. She had elevated inflammatory markers, hyperkalemia with AKI. CT chest showed bilateral lung micronodules and patchy opacity. The patient had been on long-term steroids, mycophenolate, and hydroxychloroquine. Belimumab and voclosporin were initiated after a recent kidney biopsy revealed class 4 lupus nephritis. She underwent diagnostic knee arthrocentesis and was started empirically on broad-spectrum antibiotics and antifungals. Over 48 hours, the patient developed pancytopenia and worsening hypoxia despite improving renal function. She was given pulse steroids and transferred to the ICU for elective intubation and bronchoalveolar lavage (BAL). She subsequently developed acute respiratory distress syndrome (ARDS) and bilateral pneumothorax necessitating bilateral intercostal drains. BAL returned positive for Mycobacterium tuberculosis, and antituberculosis therapy was initiated. Persistent hypoxia necessitated extracorporeal membrane oxygenation (ECMO), and worsening renal function required hemodialysis. Despite the GM-CSF, the patient had persistent severe pancytopenia and coagulopathy requiring massive transfusions. Even on ECMO she remained hypoxic and succumbed to multi-organ failure.
DISCUSSION The patient had a history of difficult-to-control lupus on long-term immunosuppressants, making both lupus flare and infection possible etiologies of presentation. Elevated inflammatory markers warranted broad antimicrobials, including antifungals. She had recently started belimumab, increasing her risk for mycobacterium reactivation. Although BAL confirmed tuberculosis, the outcome was influenced by the underlying lupus and prolonged immunosuppression. The question is, would empirical antitubercular therapy have altered the outcome? Though current guidelines require testing for only hepatitis B and C before starting belimumab, should we routinely screen for latent mycobacterium infection before starting belimumab?
-

Single-Agent and Short-Course Antibiotic Result in Optimal Outcomes for the Nonoperative Management of Perforated Peptic Ulcer
Dimitri Sagwo Tchienga, Ramon Gil, Robyn Meadows, and Shaikh Hai
-
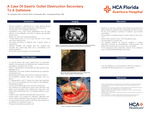
A Case of Gastric Outlet Obstruction Secondary to A Gallstone
Mahesh Tummala, Adam Devine, Akash Tummala, and Livasky Concepcion-Perez
Introduction: Bouveret syndrome is characterized by a gallstone passing through a bilioenteric fistula causing gastric outlet obstruction and represents 1-3% of gallstone obstructions. Fistualization occurs when chronic inflammation from the gallstone on the gallbladder wall leads to ischemia and perforates into the bowel. Over 60% of patients with cholelithiasis are asymptomatic. Biliary colic is the most common presentation in symptomatic patients. A biliary fistula occurs in 3-5% of cases and just 7-10% of these cases lead to gallstone ileus. The highest prevalence is among women of advanced age. Typical presentation is with general symptoms of nausea/vomiting and vague abdominal pain. Although morbidity and mortality from this condition have decreased, they remain high, likely due to comorbidities in the geriatric population. Case Presentation: Our patient is a 32 y/o female with a history of intellectual disability who presented with abdominal pain, non-bloody emesis, and inability to tolerate PO for two days. Initial CT abdomen/pelvis demonstrated gas filled structure in the gallbladder fossa. Hepatobiliary scan noted scattered intraperitoneal gas suggestive of perforated viscus. Patient began having bloody emesis and was transferred to the ICU. CT abdomen/pelvis with IV contrast was ordered and was significant for a 3x3x4 cm noncalcified soft tissue density in the duodenum. An EGD was performed as there was concern for a foreign body, and there was evidence of gastric outlet obstruction with diffuse severe ulceration of the stomach and a large ulcer with fistula in the duodenal bulb with a 3 cm impacted stone. General surgery was consulted for removal of the impacted stone. The patient underwent an exploratory laparotomy and was found to have a cholecystoduodenal fistula with gastric outlet obstruction. An open cholecystectomy, repair of the cholecystoduodenal fistula, extraction of the gallstone was performed. The patient tolerated the procedure well. Her condition improved and she was eventually discharged home.
-

Can Residents Cheat the Unknown Slide Sessions by Using the Large Language Models? Which Model Should They Use: Chat-Gpt, Claude, Or Gemini?
Gul Emek Wymer and Susana Ferra
Introduction: In recent years, artificial intelligence tools, such as large language models (LLMs) have expanded the potential for diagnostic medicine, including histopathology. This study aims to evaluate the diagnostic ability and utility of the publicly available large language models in predicting the accurate diagnosis of the unknown cases by using the images of the hematoxylin-eosin stained slides taken by a mobile phone and compare their performance with the residents’ performance.
Method: The twenty cases, including a variety of entities, were collected from teaching sets of non-HCA patients and public available domains, which are used for unknown slide sessions for residents. Three publicly available LLMs, Chat-GPT 4.0, Claude 3.5 Sonnet, and Gemini 1.5 Flash were used for generating the diagnosis of these H-E slide histology images, using a standard prompt. The same cases were evaluated blindly by four residents. The accuracy of the three LLMs were compared with each other and with the accuracy rate of the residents.
Results: The most accurate LLM was the Claude with an accuracy rate of 50%, followed by Gemini (40%) and Chat-GPT (35%). The highest accuracy rate of the LLMs (50%) was lower than the lowest accuracy rate of the residents (55%). The average accuracy rate of the LLMs was 41.66 % versus 67.5 % for residents.
Conclusions: The current LLMs are not sufficient for diagnostic use, and need to be improved for better diagnostic accuracy.
-
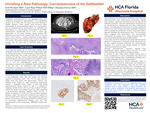
Unveiling a Rare Pathology: Carcinosarcoma of the Gallbladder
Gul Emek Wymer, Laci-Rae Pitter, and Susana Ferra
Introduction: Gallbladder carcinosarcoma is a rare and aggressive biliary tract malignancy, constituting approximately 1.7% of gallbladder cancers, with fewer than 100 cases reported in the English literature as of 2023. These tumors, often affecting gynecological organs, feature both carcinomatous and sarcomatous components. They predominantly occur in females, with a mean presentation age of 66 years. Diagnosis is primarily based on pathological analysis, and the mainstay of treatment is surgical excision.
Case Description: We present a case of an 81-year-old female with no significant medical history, who was admitted after a fall. A CT scan revealed an 18.2 cm gallbladder mass extending into the liver and colon. The patient underwent tumor resection.
Results: Pathological examination confirmed a carcinosarcoma with osteoid and cartilage elements, supported by immunohistochemical staining as gallbladder primary.
Discussion: Carcinosarcomas are composed of both epithelial (commonly adenocarcinoma) and mesenchymal (spindle cell) components. Their pathogenesis remains poorly understood. Typically diagnosed at advanced stages, these tumors have a poor prognosis, with survival rates ranging from 2.9 to 6 months. Gallbladder carcinosarcomas behave similarly to sarcomas, exhibiting rapid growth and resistance to both radiation and chemotherapy. Current treatment consensus involves surgical excision of the gallbladder, extra-hepatic bile duct, regional lymphadenectomy, and possibly pancreaticoduodenectomy depending on tumor extent.
Conclusion: Gallbladder carcinosarcoma is a rare and aggressive malignancy with a poor prognosis even following complete resection. Given the limited number of cases, further research is necessary to improve treatment strategies for these patients.