
North Texas Research Forum 2026
Files
Download Full Text (320 KB)
Division
North Texas
Hospital
Medical City Arlington
Specialty
Internal Medicine
Document Type
Poster
Publication Date
2026
Keywords
highly active anti-retroviral therapy, HAART, HIV, invasive pulmonary aspergillosis, IPA
Disciplines
Bacterial Infections and Mycoses | Internal Medicine | Medicine and Health Sciences | Respiratory Tract Diseases | Virus Diseases
Abstract
BACKGROUND: Highly active anti-retroviral therapy (HAART) has decreased the incidence of opportunistic infections among persons with HIV. Invasive aspergillosis specifically is uncommon among individuals with clusters of differentiation 4 (CD4) count >100 cells/mm3. Furthermore, treatment of aspergillosis in the HIV-infected population has not been examined systematically. We report a patient with CD4 count >200 cells/mm3, compliant with HAART therapy who developed invasive pulmonary aspergillosis (IPA) over the course of two years that was successfully treated through a combination of bronchial artery embolization and liposomal amphotericin.
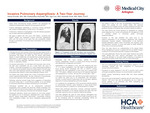
CASE PRESENTATION: A 56-year-old man from southern Africa with four-year history of HIV-1 on HAART presented to the emergency department with complaint of hemoptysis that began the same day. He denied night-sweats, fatigue, or recent weight-loss, but reported that a suspicious area was discovered on chest imaging a year earlier. He also denied any history of smoking cigarettes, significant exposure to second-hand smoke, or respiratory irritants. On physical examination patient, his vital signs and lung exam were normal. His labs were remarkable only for a white blood cell count of 4.28K/µL. Computed tomography chest imaging demonstrated a mass-like consolidation along the medial aspect of the left upper lobe which appeared severely emphysematous, with moderate emphysema also present in other areas bilaterally. He was treated with a dose of tranexamic acid and empiric piperacillin/tazobactam.
He underwent a bronchoscopy, which identified a 5 cm lesion from which aspiration and biopsy samples were obtained. The pathology report revealed fungal forms suggestive of Aspergillus and blood fungitell assay was positive. He was treated with liposomal amphotericin B. He had persistent hemoptysis and subsequently underwent angiography which revealed abnormal vessels emanating from both the right and left bronchial arteries supplying the left upper lung and these were selectively embolized. Subsequent laboratory results were positive for urine strep antigen, but negative for detectable HIV-1 load, QuantiFERON-gold tested tuberculosis, Coccidioides antibody, urine Histoplasma antigen, and serum Aspergillus galactomannan antigen.
CONCLUSION: U.S. guidelines for management of IPA recommend starting patients on voriconazole. We present a case of IPA with HIV-associated emphysema in a patient from outside the U.S. treated initially with liposomal amphotericin B to mitigate concern for azole resistance and treated later with guideline-directed voriconazole after consulting resistance patterns.
LESSONS LEARNED: Management of nonnative patients with fungal infections should account for resistance patterns internationally. However, true prevalence of resistance in the US is unknown since routine antifungal susceptibility testing is not recommended.
Original Publisher
HCA Healthcare Graduate Medical Education
Recommended Citation
Woods, Jason; Sureddi, Padmaditya; Van, Nga; and Ford, Danielle, "Invasive Pulmonary Aspergillosis: A Two-Year Journey" (2026). North Texas Research Forum 2026. 22.
https://scholarlycommons.hcahealthcare.com/northtexas2026/22
Included in
Bacterial Infections and Mycoses Commons, Internal Medicine Commons, Respiratory Tract Diseases Commons, Virus Diseases Commons

