
North Texas Research Forum 2026
Files
Download Full Text (712 KB)
Division
North Texas
Hospital
Medical City Arlington
Specialty
Internal Medicine
Document Type
Poster
Publication Date
2026
Keywords
pulmonary embolism, iliac artery aneurysm, May-Thurner Syndrome, MTS, deep vein thrombosis
Disciplines
Cardiology | Cardiovascular Diseases | Congenital, Hereditary, and Neonatal Diseases and Abnormalities | Internal Medicine | Medicine and Health Sciences
Abstract
Background: Venous thromboembolism (VTE) is a major cause of global morbidity and mortality. May-Thurner syndrome (MTS) is an iliofemoral venous compression syndrome caused by extrinsic compression of the left common iliac vein (LCIV), classically by the right common iliac artery at the level of the fifth lumbar vertebra. Although the estimated anatomic prevalence ranges from 18-49%, only 2-5% of cases are diagnosed during evaluation for lower-extremity deep vein thrombosis (DVT). Clinical manifestations range from asymptomatic venous compression to unilateral leg swelling, venous insufficiency, and acute iliofemoral DVT, with pulmonary embolism (PE) reported infrequently.
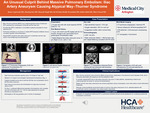
Case presentation: A 75-year-old man with hypertension, hyperlipidemia, rheumatoid arthritis, and a remote postoperative DVT presented with acute-onset dyspnea. CT pulmonary angiography revealed a massive, occlusive PE involving the right main and left pulmonary arteries with evidence of right heart strain. Lower-extremity venous duplex USG showed extensive left iliofemoral DVT. Subsequent CT angiography of the abdomen and pelvis identified aneurysmal dilation of the LCI artery with associated mural thrombus, resulting in extrinsic compression of the adjacent LCIV, consistent with an atypical variant of MTS. Given a high Pulmonary Embolism Severity Index score (115), the patient underwent percutaneous mechanical aspiration thrombectomy for PE. On hospital day three, staged left lower-extremity mechanical aspiration thrombectomy was performed, followed by angioplasty and venous stenting with a 16 × 150 mm Abre venous stent. Post-dilation with a 16 × 40 mm balloon and intravascular ultrasound (IVUS) confirmed full stent expansion, appropriate wall apposition, and restoration of luminal flow. The patient was discharged on apixaban for at least six months and clopidogrel for two to three months. At follow-up, he subsequently underwent elective endovascular repair of the left common iliac artery aneurysm to prevent further progression.
Learning points: MTS should be considered in patients with recurrent venous thromboembolism despite minimal or absent symptoms. Diagnosis relies on multimodality imaging, with venous duplex USG as the initial screening tool and venography with IVUS as the reference standard for definitive anatomic assessment. Management strategies are guided by symptom burden and thrombotic complications. Asymptomatic or mildly symptomatic patients are typically managed conservatively, whereas symptomatic disease warrants an individualized endovascular approach. Anticoagulation following venous stenting should be tailored to thrombotic risk factors and overall clinical presentation.
Conclusion: MTS may represent a provoked cause of pulmonary embolism despite negative hematologic evaluation, warranting timely recognition and early management.
Original Publisher
HCA Healthcare Graduate Medical Education
Recommended Citation
Lapsiwala, Boney; Xue, Jiaming; Singh, Mayank; Reddy Dronadula, Sai Krishan; Zahid, Sadia; and Yousef, Mian, "An Unusual Culprit Behind a Massive Pulmonary Embolism: Atypical May-Thurner Syndrome from Iliac Artery Aneurysm" (2026). North Texas Research Forum 2026. 24.
https://scholarlycommons.hcahealthcare.com/northtexas2026/24
Included in
Cardiology Commons, Cardiovascular Diseases Commons, Congenital, Hereditary, and Neonatal Diseases and Abnormalities Commons, Internal Medicine Commons

